Yener Demirtas, MD, Suhan Ayhan, MD, Yakup Sariguney, MD, Fulya Findikcioglu, MD, Osman Latifoglu, MD, Seyhan Cenetoglu, MD, and Cemalettin Celebi, MD.
Introduction: Although the current argument regarding reduction mammoplasty is essentially concentrated on reducing the scars and improving the cosmetic results, many plastic surgeons are still engaged in efforts to minimize bleeding and drain requirement in breast surgery. Breasts are well known to show cyclic changes in accordance with menstrual cycle. Speculations have been made on ideal timing of breast surgery in this extent, but the clinical evidence to support their global acceptance and application is lacking. This study was designed to establish the relationship of intraoperative bleeding and postoperative drainage with the menstrual period of the reduction mammoplasty patient.
Material and Methods: Thirty-five otherwise healthy patients scheduled for bilateral reduction mammoplasty were included in this prospective study. Operations were performed by the same surgical team who had no information concerning the menstrual histories. Data were collected postoperatively and were used to group the patients as perimenstrual, periovulatory and postmenopausal. Inferior pyramidal technique under standard general anesthesia was used and each breast was infiltrated with 20 ml of 1% lidocaine and 1:160000 adrenaline prior to surgery. Intraoperative blood loss was calculated by soiled swab technique. Postoperative drainage was collected for 72 hours using standard silicone drains.
Results: Sixteen patients were in the perimenstrual phase (Group 1: day 0 to 7 and 21 to 28) and 13 in the periovulatory phase (Group 2: day 8 to 20). The mean ages of the patients and the average weights of the tissue resected per breast were insignificant between these groups. Six patients were in the postmenopausal period (Group 3). Overall, there was only one case of a T-junction breakdown as early postoperative complication. Mean intraoperative blood loss and postoperative 72 hours drainage per patient were 146,1 and 175 ml in Group 1, 68,6 and 125 ml in Group 2 and 56,8 and 140 ml in Group 3, respectively (Fig. 1 to 3). The difference between Groups 1 and 2 was statistically significant for both of the parameters (p<0,05).
Conclusions: The results of this study indicate that both perioperative blood loss and postoperative drainage are significantly reduced when breast reduction is performed in periovulatory phase compared with perimenstrual phase. We strongly recommend the interval between days 8 and 20 of menstrual cycle as a more convenient period to perform a breast reduction. The drains may be avoided in this period, but they would rather be preferred if the surgery is done in the perimenstrual phase.
| |
| | 
|
Figure 1: Intraoperative blood loss of the patients versus the day of menstrual cycle at the time of surgery. | |
| | 
|
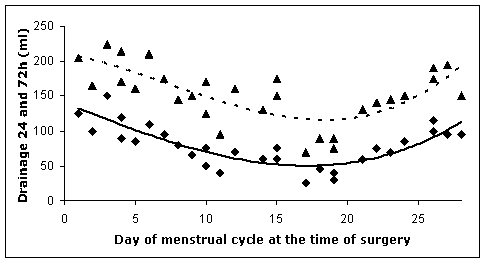
Figure 2: Postoperative 24 hours ( ) and 72 hours (
) and 72 hours ( ) drainage of the patients versus the day of menstrual cycle at the time of surgery.
) drainage of the patients versus the day of menstrual cycle at the time of surgery.
| | 
|
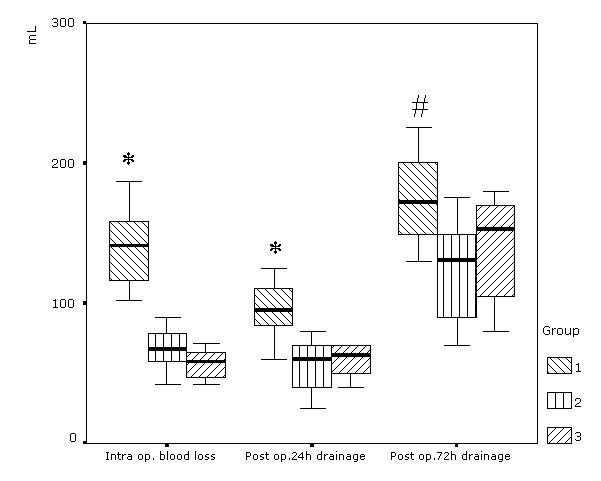
Figure 3: Comparison of intraoperative blood loss and postoperative drainage between groups. Statistical significance (p < 0.05) as indicated: *p < 0.001 vs. group 2; #p = 0.002 vs. group 2.



