Sunday, October 10, 2004
6024
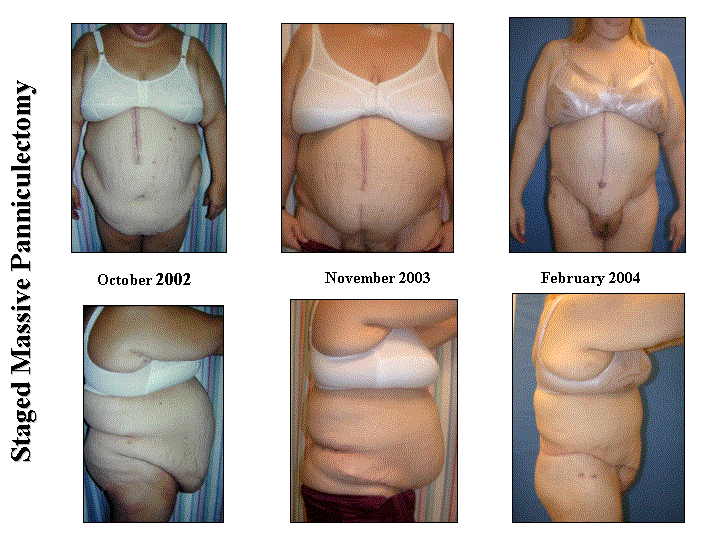
Massive Panniculectomy after Massive Weight Loss
Purpose: Obesity is a disease steadily increasing in incidence and prevalence, affecting all age groups and ethnicities. The medical complications of obesity are well known. Dramatic weight reduction achieved through diet and exercise or surgery can reverse morbidity and mortality associated with obesity. Sequelae of massive weight loss include skin redundancy and fascial laxity, particularly in the abdomen. The abdominal pannus causes disabling rashes, pain, physical limitation, back strain, and cosmetic deformity, and symptoms are more marked the heavier the pannus. Panniculectomy can treat these symptoms, but the approach must be customized due to complex medical and surgical histories related to obesity and the size of the pannus. The aim of this study was to analyze a series of massive panniculectomies greater than 10 pounds following massive weight loss to better characterize the patients receiving these procedures and the outcomes achieved. Methods and Materials: All patients undergoing massive abdominal panniculectomy by a single surgeon at an academic hospital from October 2000 to December 2003 were retrospectively studied. Seven men and 17 women qualified: 1 woman had a 2 stage abdominal panniculectomy, each time with greater than 10 lb abdominal skin resections. All but 1 patient had gastric bypass. Average weight loss was 171 lb, with average maximum BMI of 70.5, and minimum BMI of 43.7. (Morbid obesity = BMI > 35) Patient presentation was regularly complicated by upper midline incisional hernias with adherent scar, and abdominal scars from unrelated previous surgery including subcostal incisions. Abdominal panniculectomy was performed with conservative undermining, often assisted by suspending the skin from ceiling chains. Hernias were repaired at the time of surgery by approximation and plication of the fascia. Lax fascia was plicated as well. Closure of the skin was performed in a layered fashion over 2 to 4 Jackson-Pratt drains. Ambulation was encouraged within 24 hours of surgery. Results: Average abdominal skin resection was 16.1 lb, ranging from 10.3 to 49 lb. Hernia repair was necessary in 13 patients, and mesh was not used in any patient. Additional surgery performed at the time of panniculectomy included skin reduction surgery of the back (40%), chest (32%), inner thigh (28%), and arm (28%). Blood transfusion was necessary in 5 (20%) of the cases. Length of stay averaged 3 days. Complications included wounds requiring debridement, dressings, VAC therapy and/or delayed primary closure (20%); and seroma requiring drain replacement or dressings (28%). Uncomplicated healing occurred in 44% of cases. There were no DVT’s or mortalities. Conclusions: Massive abdominal panniculectomy is challenging to plan, execute and manage after surgery. We present our approach to these patients with acceptable results.
View Synopsis (.doc format, 183.0 kb)