Suhan Ayhan, MD, Yener Demirtas, MD, Osman Latifoglu, MD, and Kenan Atabay, MD.
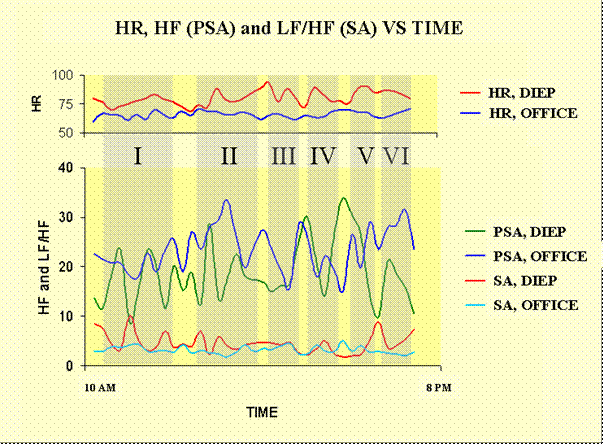
Introduction: The daily activities of all individuals encompass, from time to time, situations which are associated with heightened degrees of emotional arousal that are usually referred as “stressful”. Human body is a non-stop working machine and some units of this machine, particularly the cardiovascular system, are more vulnerable to erosive effects of psychological strain. We wanted to evaluate the mental stress of a surgeon during microsurgery, after performing similar studies on rhinoplasty and liposuction, by the aid of a recently popularized method, heart rate variability (HRV). HRV utilizes periodic fluctuations of the heart rate to assess relative contributions of parasympathetic and sympathetic nervous systems. Material and Methods: A 34 year-old male plastic surgeon was monitored with a digital Holter recorder on two occasions between 10 AM and 8 PM; during a breast reconstruction with deep inferior epigastric artery perforator flap and during a routine office day without any surgery. Heart rate and two indices of HRV (high frequency component, HF, as an indicator of parasympathetic activity and low to high frequency ratio, LF/HF, reflecting sympathetic activity) were analyzed from those recordings utilizing computerized research tool software. The analyzed data were then compared. Results: The effect of performing microsurgery on cardiac autonomic modulation of the operator was striking. Mean values and the course of the measurements are given in the table and the figure. Heart rate and sympathetic activity of the surgeon were consistently higher during DIEP when compared with office day values, and parasympathetic activity was lower during surgery. Conclusion: Surgery is a demanding job, requires absolute concentration of the operator and there happens periods of considerable tension during some operative procedures. Microsurgery is the very prototype of this kind, as our results revealed. The pure psychical stress results in cardio-circulatory and metabolic effects in the sense of an “alarm reaction”, which prepare a subsequent physical reaction without the possibility of having this reaction really performed. There is evidence that such metabolically or energetically not “consumed” stresses have negative long-term effects on human health, in such a manner that sustained psycho-physiological activation has been identified as a risk factor for development of hypertension, cardiac arrhythmias, blood lipid disturbances, diabetes mellitus, and probably coronary heart disease. Although minimal tolerance -if any- is shown for unfavorable results of surgeons, our results suggest that aroused emotional status of surgeons during an operation makes them more prone to make mistakes due to physical and mental fatigue and strain. This sympthatehic hyperactivity that might have a significant negative impact on surgeon’s performance especially on difficult and long procedures, as in the case, should be taken into consideration when their liability is concerned. This point questions whether the level of legal responsibility of surgeons can be categorized as well according to their working conditions, because operating rooms and the surgeon’s garments have been designed largely with bacteriologic or safety considerations in mind. The environmental engineering considerations have been very few, and, for the most part, operating room paraphernalia seem more apt to be a disadvantage to the operator than to improve his comfort or performance.
| | OFFICE | DIEP |
| Heart rate (bpm) | 66 ± 3 | 80 ± 6 |
| Parasympathetic activity (HF, nu) | 23.5 ± 4.5 | 18.7 ± 6.2 |
| |
| Sympathetic activity (LF / HF) | 3.2 ± 0.8 | 4.6 ± 2.0 |
| |